Brain and Spine Care
Want to learn more about this at Kettering Health?
At 13 years old, Shannon Gavin was diagnosed with epilepsy. Fifteen years later, despite medication, she continued to suffer from recurring seizures. But at a checkup in January 2023, William Gebele, a physician assistant, recommended a stay in the Epilepsy Monitoring Unit (EMU) in the hopes of a more permanent solution.
Looking for crucial information
It might seem complicated, but the EMU, located at Kettering Health Main Campus, has one basic purpose.
“We determine where a patient’s seizures are coming from,” says Brandy Magnaterra, a registered electroencephalogram (EEG) technician.
In the EMU, technicians place electrodes on a patient’s scalp to monitor their brainwaves, a diagnostic test known as an EEG. This monitoring allows technicians and epileptologists to determine the location of a patient’s seizures, which helps them understand the type of seizure someone is having.
This information, then, helps them decide what medication would be best to try and whether the patient is a candidate for surgery. Shannon hoped to be one of these eligible patients.
A shocking discovery
Experiencing several large seizures a year made everyday life—driving and working—difficult or nearly impossible for Shannon.
“When you’re 28 years old,” she says, “it’s hard to realize you can’t do everything other people do.”
She was hesitant to take a week away from her life to stay in the EMU. But she knew she made the right decision after learning shocking news about her condition.
24/7 monitoring
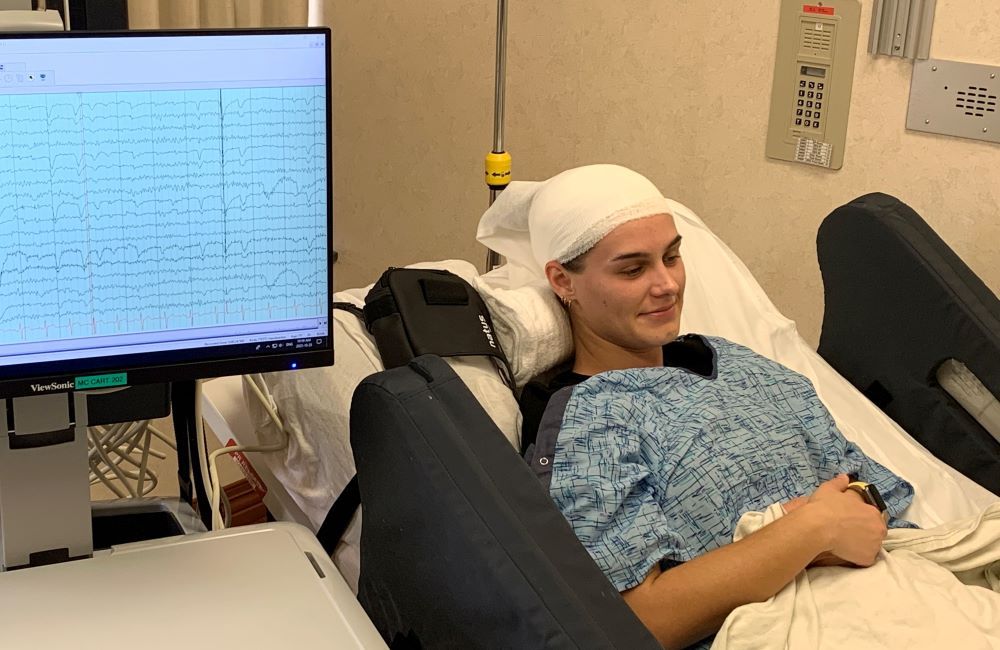
Patients are continuously monitored in private rooms for up to five days in the EMU. In a separate room, a dozen monitors show each patient’s brainwaves and live video captures any physical changes.
While an EEG might look like random lines to the untrained eye, for EEG technicians, the monitors reveal where activity is occurring in the brain. In other words, they can tell where a patient’s seizures are coming from. They can also see small spasms in the brain, known as electrical discharge, which Brandy says, “means they’re at risk for having a seizure.”
It’s this continuous monitoring that makes the EMU so beneficial. A typical EEG monitors someone only for a short time, usually no more than an hour, and they may not have a seizure. Even an ambulatory EEG, which the patient wears at home for one to three days, might not capture enough helpful information. The EMU, however, allows for around-the-clock monitoring in a controlled environment.
Through this 24/7 monitoring, Shannon, who thought she had only a handful of seizures a year, found out she actually had up to 45 seizures a day.
Shannon’s solution
The EEG gave her team a good idea of where the seizures were happening. But they needed to pinpoint the exact location if Shannon was going to have a focal resection—a surgery to remove the part of the brain responsible for someone’s seizures.
To do this, Nuclear Medicine technicians needed to inject radioactive dye into Shannon’s brain during one of her larger seizures. The dye would then bind to receptors in Shannon’s brain at the site of her seizure, narrowing the location during an ictal single-photon emission computed tomography (SPECT) scan, a type of nuclear imaging test that shows how blood flows to tissues and organs.
On the last day of Shannon’s EMU stay, the technicians were able to inject the dye during a seizure and capture the needed information.
With this information, Dr. Mark Hoeprich, a neurosurgeon, and Dr. Taylor Kabacinski, Shannon’s epileptologist, decided on phase 2 of Shannon’s treatment. Dr. Hoeprich surgically placed depth electrodes in her brain where her seizures were happening. During another stay in the EMU, these depth electrodes pinpointed Shannon’s exact seizure location.
She’s since moved on to phase three—resection surgery—and is one step closer to becoming seizure-free.